A treatment that has been known in Eastern Europe for over 70 years could be the answer to
Antibiotic Resistant Infections.
Antibiotic Resistant Infections.
|
Infections due to the MRSA bug continue to cause concern in many hospitals in the U.K and other bacteria such as Clostridium Difficile are beginning to alarm doctors because of their increasing resistance to treatment with antibiotics. Today’s escalating antibiotic crisis is the direct result of large scale and indiscriminate over-use of anti-infective drugs and now pharmaceutical companies have exhausted the arsenal of known antibiotic classes. Currently, the launch of new antibacterial products usually includes stronger dose formulations of old antibiotic classes. This results in the development of more antibiotic resistant strains and increased resistance of current strains.
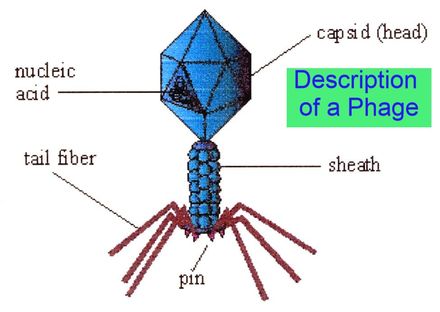
PHAGE THERAPY TO THE RESCUE However, a technique called “phage therapy” could be the answer. This therapy uses viruses that infect and kill bacteria. It offers a new and effective weapon to combat infectious diseases for both resistant and sensitive bacteria strains. In Eastern Europe phage therapy has been routinely used to treat a wide range of bacterial infections for over 70 years with excellent results. This technique of using of bacteriophages, or “bacteria-eaters”, was pioneered in the former Soviet Union at around the same time as the discovery of antibiotics, which were much more swiftly effective. Although penicillin and other such drugs changed medicine, one team in the Georgia Eliava Institute of Bacteriophage, Microbiology and Virology in Tbilisi continued to research phages. The demise of Communism and the Georgian civil war of the early 1990s was a disaster for the Institute, which saw the loss of most of its phage collections, the collapse of its infrastructure and subsequently the relocation of phage research and production to Russia. VIRUSES EXTRACTED FROM RAW SEWAGE The word bacteriophage was coined in the 1920s by French-Canadian microbiologist Felix d’Herelle who, while investigating an outbreak of dysentery in Paris, discovered that a surprising variety of infections could be cured with the aid of viruses extracted from raw sewage. One-fortieth the size of bacteria, these viruses are found wherever bacteria thrive, in oceans, in our bodies and above all in sewage. They have an extra-terrestrial look, with large heads, narrow tails and spidery legs. They inject their prey with their offspring, which multiply so fast that the host literally bursts. The beauty of phages is that, unlike antibiotics, they can mutate to keep pace with the bacteria they are programmed to destroy, developing new modes of attack as the bacteria become resistant to them. Their limitation lies in the fact that each can act on only one specific host. No wonder they were upstaged in the West by antibiotics, which kill everything in their path. RESEARCH IN GEORGIA WAY IN ADVANCE However, in the East this was not the case. Way back in 1923 when the Georgian scientist, George Eliava, founded the Institute in Tbilisi it was devoted to the ideas of d’Herelle who had settled in the Soviet Union. The Institute researched new remedies and exported them to every corner of the Soviet Empire. They were generally used as alternatives to antibiotics, as they still are in Tbilisi, now in the Republic of Georgia, but they were also often used in tandem. Up until a few years ago Western medical culture had been unaware of phage therapy’s considerable achievements in the former Soviet Union owing to a variety of historical, political and bureaucratic circumstances. Hardly any of the numerous Russian language publications have been translated into English, let alone reviewed. |
VIRUS LIBRARIES
Because each phage is specific to a particular bacterium this could present a problem as scientists would have to build up virus libraries to have an effective weapon against infections. They would then have to do detailed tests on patients to ensure that they used the correct virus and this could delay the start of the treatment. In the treatment, doctors flood the patient’s bloodstream with the virus, a simple entity made of a protein envelope carrying genetic instructions inside. When the virus lands on the bacterium, it injects its genetic material into it and the bacterium is fooled into thinking that the material is part of its own genetic instructions. Unfortunately for the bacterium, the virus instructs it to produce many more viruses that build up inside it until it explodes and dies. BIGGEST MEDICAL BREAKTHROUGH IN DECADES According to Dr.James Soothill, a microbiologist at Manchester University who forecast the present crisis with antibiotics some years ago, one of the advantages that phages have over antibiotics is their ability to replicate at the place in the body where you want them. They constantly evolve and can adapt in situe to resistant bacteria strains. He said, “they don’t simultaneously kill most of the body’s normal, helpful bacteria and they can multiply from one to tens of billions in a mere five hours.” In fact phages actually support and enhance vital microflora in contrast to the indiscriminate action of wide-spectrum antibiotics, which can decimate the body's protective normal microflora. It is claimed that phages can cure dysentery, septicaemias, some forms of meningitis and have also been effective against epidemic cholera. Because of the phages' extreme specificity and chemically large nature, they have induced no side or adverse effects when used as a therapy in clinical practice, nor do they affect the body's natural immune system. Microbiologist Dr. Paul Barrow who is one of the few British experts on phage technology, believes that phages could offer the biggest medical breakthrough for decades, but he says, “money would have to be committed to it…..millions have been invested recently in a new vaccine research centre, but virtually nothing is being done to support research into phages. It’s a crazy situation.” PHARMACEUTICAL COMPANIES RELUCTANT TO INVEST Production costs of phages are actually quite low but pharmaceutical companies have been reluctant to put money into phage research because they have heavily invested in chemical antibiotics and without a patentable end product, development is not commercially viable. However, phages present virtually the only possible alternative and, potentially, the last resort for the treatment of antibiotic-resistant pathogens. Despite a general disregard for Russian research and clinical practices in the West, phages have been used safely in Georgia, Russia and Poland for many years but Western medical authorities are less enthusiastic and physicians may be reluctant to forego wide-spectrum antibiotics in favour of the highly specific phages. DYING PATIENTS SAVED BY PHAGE THERAPY The first person in the West to be cured of a bacterial infection by phage therapy is believed to have been in September 1999 when, according to a report in the Guardian newspaper, a company in Seattle, which had taken up the technique, cured a Canadian woman of a bacterial infection by the use of a virus. A spokesman said, “The woman was going to die: she had an antibiotic-resistant infection so they used a phage therapy and it saved her life”. More recently, Tom Patterson, a professor in the Department of Psychiatry at UC San Diego School of Medicine, became infected with a multidrug-resistant strain of bacterium in late 2015 while holidaying in Egypt with his wife. Within three days of starting the phage therapy, the patient, who was near death emerged from his coma. Some months later, the bacteria were found to be no longer present in his body and he was able to go back to work. As a result of this unprecedented success, the San Diego medical team envisage opening a centre specially dedicated to bacteriophage research in the aim of advancing research and development of phage-based therapies. URGENT ACTION NEEDED As the spread of antibiotic resistance reaches crisis point, the window of opportunity for phage therapy is at last being re-opened in the West. Medical experts anticipate record increases of anti-bacterial resistance in the next decade, so action must be taken now if we are to stop the onslaught of dangerous bacteria that is causing havoc in our hospitals. It is critical that the world’s weapons against superbugs are augmented as soon as possible. There is no time to lose. |
The World Health Organization estimates that antimicrobial resistance could kill at least 50 million people per year by 2050 with an economic cost of trillions..